Each year, the federal government updates the Federal Poverty Level (FPL). These guidelines help determine eligibility for many public assistance programs.
In California, the FPL plays an important role in health coverage eligibility. It helps determine whether individuals and families qualify for Medi-Cal, Covered California premium subsidies, and enhanced Silver health plans.
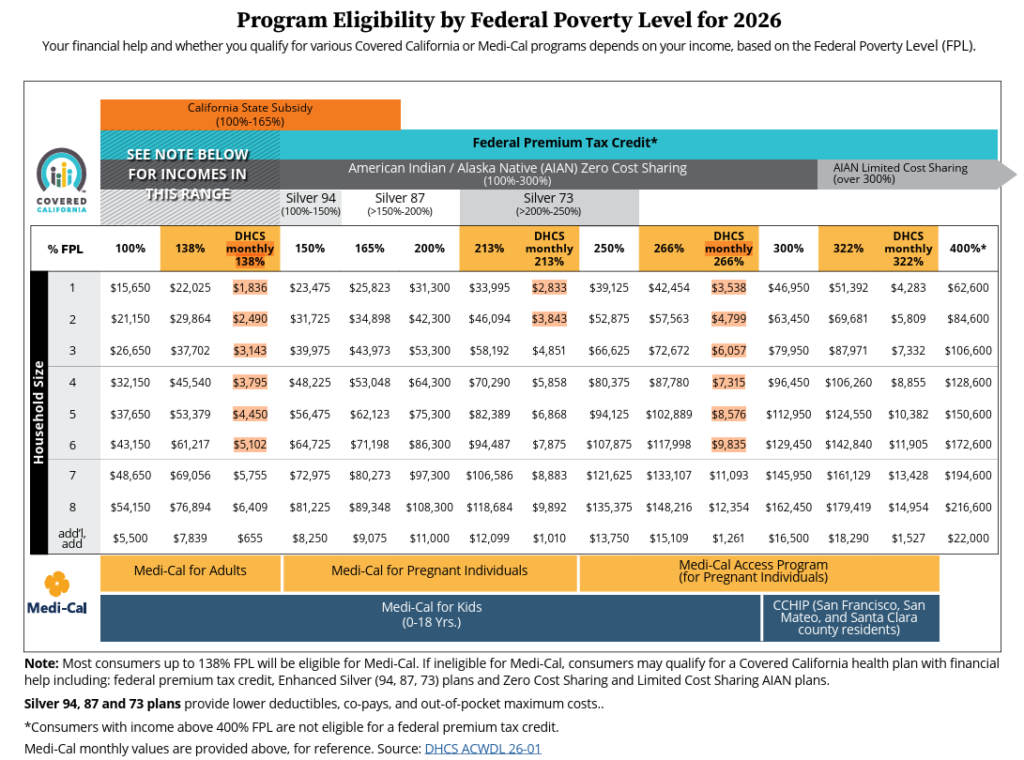
For the 2026 coverage year, the poverty benchmark is $22,045 for a single individual and $45,540 for a household of four.
Covered California and Medi-Cal use these baseline numbers to calculate income percentages such as 138%, 200%, or 400% of the Federal Poverty Level. These percentages determine eligibility for different health coverage programs and financial assistance.
Understanding where your household income falls relative to these thresholds is essential when applying for health insurance or estimating subsidy eligibility.
How Household Income Is Calculated
Eligibility for Covered California subsidies and Medi-Cal is based on Modified Adjusted Gross Income (MAGI).
MAGI generally includes:
- Wages and salaries
- Self-employment income
- Unemployment benefits
- Certain Social Security income
- Investment income
Many individuals review line 11 on their federal tax return. As a result, they use this number as a starting point to estimate next year’s income for subsidy eligibility.
Household size is determined by the tax household. Specifically, it includes individuals listed on the same federal tax return.
Why the Federal Poverty Level (FPL) Matters
Even small changes in household income can affect eligibility for:
- Medi-Cal coverage
- Covered California premium subsidies
- Enhanced Silver plans
- California state financial assistance
Because of these income thresholds, accurately estimating income during enrollment is critical to avoid unexpected tax repayment or missed subsidy opportunities.
Medi-Cal Redetermination Process
Medi-Cal redetermination (also known as renewal or recertification) is when the state reassesses a person’s eligibility for Medi-Cal. Covered California may automatically renew some individuals based on information from tax returns, bank statements, or other government assistance records such as SNAP benefits or unemployment. Others may need to submit additional documentation to confirm eligibility.
Medi-Cal beneficiaries will receive renewal notifications by mail or email from their state Medi-Cal agency. Therefore, it is important to update your contact information with the state agency and respond within the 60-day deadline to avoid losing coverage.
Understanding health insurance eligibility rules can be challenging, especially as income thresholds, subsidy formulas, and program requirements change each year.
If you have questions about your estimate income for subsidy eligibility, compare Covered California plan options, evaluate Medi-Cal qualification, and understand enhanced Silver plan benefits, please contact Solid Health Insurance Services at 310-909-6135 or email info@solidhealthinsurance.com.
At Solid Health Insurance Services, we help you choose health, dental, vision, life, and long-term care coverage that supports your well-being and fits your budget.
