States are preparing to remove millions of people from Medicaid as protection coverage enacted during the COVID-19 pandemic will expire. In California, the state welfare program is called Medi-Cal and not Medicaid, as it is called in the other states. The upheaval, which will begin this April, will put millions of low-income Americans at risk of losing health coverage, threatening their access to care and potentially exposing them to huge medical bills. Not only that, it will put pressure on the finances of hospitals, doctors, and others relying on payments from Medicaid, the state-welfare program that covers lower-income people and people with disabilities (Medi-Cal in California).
Almost three years ago at the beginning of the Covid-19 pandemic, the federal government agreed to send billions of dollars in extra Medicaid funding to states on the condition that they keep people enrolled in Medicaid.
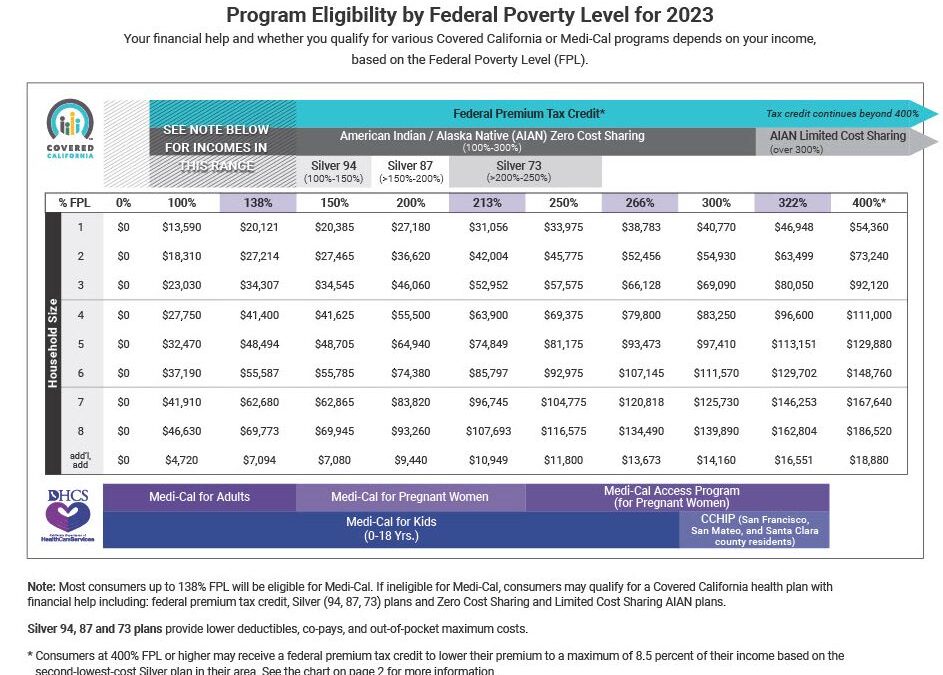
As a part of the Consolidated Appropriations Act of 2023, California and other states will resume disenrolling people who do not qualify for Medi-Cal and connect them to Covered CA and other programs as the states phase down the enhanced federal Medicaid matching funds.
The Biden Administration has predicted that 15 million people, or 17% of enrollees, will lose coverage through Medicaid or CHIP as the programs return to normal operations. The challenges are steep because it has to be ensured that they do not disenroll people who are still entitled to Medicaid. Even before the pandemic, the states struggled to reach out to Medicaid recipients. In California, it is estimated that approximately 2 million California will be disenrolled from Medi-Cal.
Medicaid Redeterminations
Medicaid redetermination (also called renewal or recertification) is a process where states redetermine an individual’s eligibility for Medicaid. Medicaid redetermination was paused in early 2020 due to the Covid-19 public health emergency (PHE). With the passage of the recent legislation, the states will resume the redetermination process and will end coverage for individuals who are no longer eligible. Starting April 1, 2023, states will begin the recertification process and have until May 24 to recertify their members.
Some individuals may be automatically renewed by their Medicaid agency based on the information the state uses to confirm eligibility (e.g., tax returns, bank accounts, unemployment, SNAP eligibility) Others may need to take action and provide documentation to verify their Medicaid eligibility. Beneficiaries will be notified by their state Medicaid agency via postal mail or email when they are having their overage redetermined. It’s important that members have their current contact information on file with their state agency. It is imperative to respond within the 60-day time frame provided so beneficiaries will not lose their coverage.
When notified, beneficiaries may need assistance understanding what they need to do. One of the carriers, United Healthcare (UHC) took an initiative to offer members through the redetermination process. There will be an outbound call and direct mail for most D-SNP members. UHC will send letters to their members should they fall for the redetermination process and ask these members to provide authorization for the recertification process.
If you have questions about how to obtain Covered California health insurance or any other medical health insurance, please contact us at Solid Health Insurance Services. We will find you a health insurance plan which is affordable and meets your insurance needs.